.
.
.
.
We are thrilled to announce that the APGI has once again bought together the expertise of clinicians and scientists around the country to map the genetic underpinnings of a rare type of Pancreatic Cancer- Pancreatic Neuroendocrine Tumours (PNET), published in Nature Today.
Neuroendocrine tumours (NETs) is the umbrella term for a group of unusual, often slow-growing cancers. These tumours develop from secretory cells found throughout the body and which are particularly concentrated in the gastrointestinal system, lung, pancreas, ovary and testes. We don’t often hear about these types of tumours as they represent only 2% of all Pancreatic Tumours diagnosed in Australia. Neuroendocrine tumours of the pancreas are a distinct subtype of pancreatic tumour – they are made up of the cells that are responsible for producing hormones, several of which control blood sugar in the body, such as insulin. Many people don’t know that pancreas has 2 important functions and is made up of 2 different types of cells: the endocrine cells make several kinds of hormones, such as insulin, and the exocrine cells make enzymes that are released into the small intestine to help the body digest food. This dual function makes the pancreas an absolutely vital organ.
This is the type of tumour that the man who introduced us to the iPhone 10 years ago, Steve Jobs, died from in 2011.
Pancreatic NETs fall into a challenging spectrum of those that are slow growing and behave predictably, and respond to treatments such as surgery or chemotherapy drugs. But others behave very differently. They can be aggressive, spread to other parts of the body and be highly resistant to many treatments. There is no one screening tool or diagnostic marker that can reliably be used to test for these tumours.
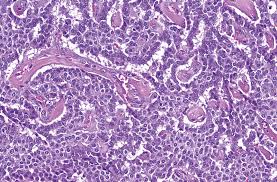
Herein lies the problem
If you were diagnosed with a Pancreatic NET today, your doctor may not know up-front which category your tumour would fall into- whether it would grow slowly or be one of the more aggressive types. They may not know whether you require chemotherapy treatment, and if you did, whether you would benefit from this treatment. There is a lot at stake here: long-term survival and quality of life often depend on the clinical choice of therapy.
The discovery may be ground-breaking: but what does this mean for patients?
Thanks to many of our dedicated clinicians at Royal North Shore Hospital (Professor Jas Samra), Bankstown Hospital (Professor Neil Merrett), Fremantle Hospital (Dr Krishna Epari and Dr Mo Ballal), and Princess Alexandra Hospitals (Dr Jonathan Fawcett and Dr Tom O’Rourke) and their generous patients we were able to collect tumour samples and perform highly specialised genomic sequencing techniques on them to decrypt the genetic landscape of these tumours. National leaders in cancer genomics, and APGI Leadership Team members Professor Sean Grimmond from the University of Melbourne, and Dr Nic Waddell from QIMR Berghofer Medical Research Institute lead the data analysis component. Global contributions from colleagues at the University of Verona in Italy and Baylor College of Medicine in the USA were crucial to ensuring this was the largest cohort of PNET’s ever analysed in this way. We found PNETs had a lower overall rate of genetic faults compared to cancers of the exocrine cells (Pancreatic Ductal Adenocarcinomas), which means we have a fine-tuned list of targets to hone in on. Among the key findings were 2 important points emerged that have never been reported in these tumours previously:
Firstly, inherited mutations were uncovered. It has been thought that only 5% of these tumours were caused by hereditary factors related to conditions of increased risk due to mutations of the MEN1 or VHL gene. The study revealed that as many as 17% of the cases were linked to inherited mutations, not only of these two known genes, but also due to other genes more well known for their role in breast, ovarian and colon kcancers, such as the CHEK2 and BRCA2 genes. Importantly you don’t need family history of cancer to potentially carry a faulty gene that may increase your risk of developing this tumour. This will require us to think differently about the way we assess and manage familial risk in this type of tumour.
Secondly, aggressive behaviour was identified by a particular genetic fault, which was previously only found in rare tumours of the soft tissue including the type called Ewing Sarcoma. This is a promising avenue to develop, as it gives us predictive power up-front to determine the aggressive behaviour of individual PNETs and which may require decisive therapy.
We now have more insight into how we may predict the aggressiveness of individual tumours at the time of diagnosis who may benefit most from treatment, and avoid unnecessary treatment for those whose tumours may behave in a more predictable way.
Thanks to all out patients and families who contributed to this study. Thanks also to our clinicians and scientists for everything you do for our patients, and your commitment and continued collaboration on this very important work.You can read the full media release here.
